
The Costs of Variation in Healthcare: A Closer Look at Test Ordering Patterns
In 1785, William Cowper penned “The Task,” a poem in which he used the phrase “variety is the spice of life.” Since that time, the expression has been frequently used to express the concept that new and exciting things make life more interesting. The expression continues to be used, at least in part, because people find that to be true.
Although variety in healthcare can make things more exciting, there is also a downside that needs to be considered.
Variation, or variety, introduces complexity in healthcare, resulting in significant negative consequences for patients, providers, and payers. With the increasing focus on individualized medicine, it seems logical to conclude that variation/ variety is simply an expected part of the diagnostic and treatment process. Some variation is certainly even desirable, but the degree of variation commonly present in healthcare is not and can lead to undesirable outcomes.
What are some examples of such variation?
Reducing Test Ordering Variation
Use of services delivered by the clinical laboratory is an excellent example of a place within the healthcare ecosystem that shows considerable variability in ordering patterns for patients with the same major condition/disease.
For example, the graph below shows the frequency distribution for unique tests ordered by a number of providers caring for patients being evaluated for chest pain.
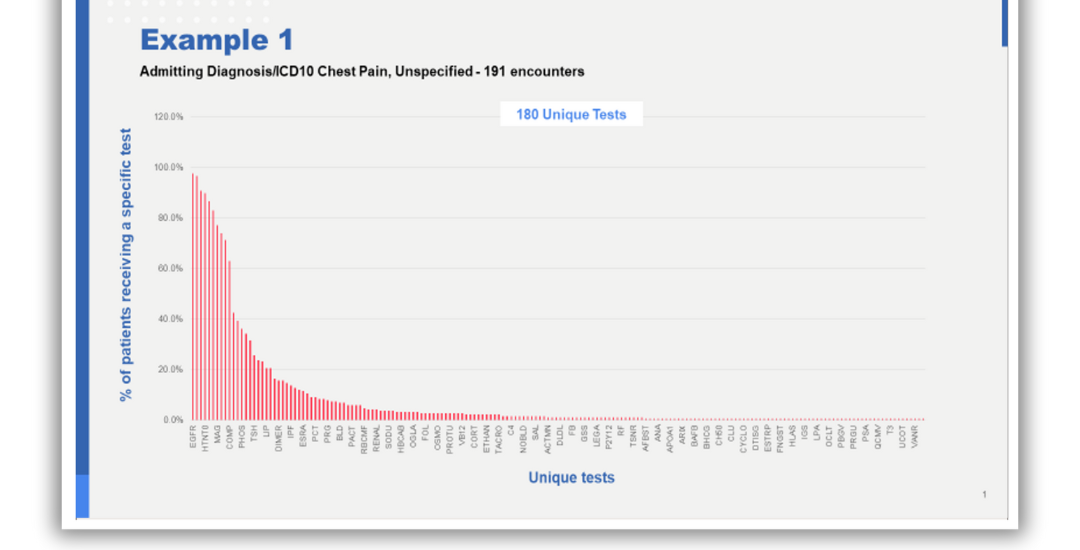
Source: Deidentified and anonymized CareTinuum Advisors data
In this example, providers collectively ordered 180 unique tests for the 191 patients that were being evaluated for chest pain. Not all of these patients were indeed identical. Some had comorbid conditions and were, therefore, being evaluated for multiple complaints/issues at the same time. That fact contributes to a portion of the variation seen.
However, none of the tests were ordered 100% of the time, and many of the tests were ordered very infrequently. There is significant variation in the ordering patterns for this group of patients being evaluated for the same primary complaint. We have observed this ordering pattern variation on numerous occasions involving multiple health systems and concerning a variety of clinical situations.
Tackling Test Result Variability
So, what is the problem with this variation, and why isn’t it just the “spice” of medical evaluation? In part, the answer to that question lies with the impact of the results of testing on the subsequent evaluation of the patient.
Most laboratory tests have a normal range defined by the mean plus or minus two standard deviations for a group of patients without disease/complaints. This definition means that 5% of individuals without complaints will have a result outside of the normal range.
Providers commonly try to explain such abnormal results; they often order additional laboratory tests or imaging studies to rule out a condition that could be associated with a statistically driven incidental abnormal test result. This scenario gets even more complicated when a large number of tests are ordered as a part of the initial evaluation of a patient.
In short, the variability introduced in the ordering pattern has the potential unintended negative consequence of leading to additional downstream costs for patients and payers.
As described in a JAMA Open Network article in 2019*, care cascades resulting from incidental clinical laboratory findings are common and may prompt testing and treatments that are of uncertain value.
Over eighty-six percent of the physicians (86.7% of study participants) in the study reported issues with care cascades triggered by imaging 55% of the time, blood tests 35% of the time, and cardiac, urine, stool, microbiology, and pathology tests making up the remaining 10% of the events.
The physicians reported that these issues caused their patients and themselves the following types of harm:
- Psychological harm – 68.4%
- Treatment burden – 65.4%
- Financial burden – 57.5%
- Dissatisfaction with care – 27.6%
- Physical harm – 15.6%
Physicians reported they personally experienced:
- Wasted time and effort – 69.1%
- Frustration – 52.5%
- Anxiety – 45.4%
So, how can we keep what is good about individualized, patient-centric care and still reduce the variability that can have negative consequences?
Optimizing Diagnostic Guidelines
One approach that has been used is to develop practice/diagnostic guidelines. Such guidelines are based upon real-world data and the experience of key opinion leaders and specialists.
Organizations such as the Institute for Clinical Systems Improvement have championed the development of guidelines for many common clinical situations.
The U.S. Preventive Services Task Force has also published guidelines primarily related to delivering preventive services.
Most of these efforts have logically focused on the clinician/provider, and a few of the services delivered by the clinical laboratory are included in the guidelines.
Given the fact that approximately 70% of the objective data upon which clinical decisions are made come from the clinical laboratory, and in light of the potential unintended negative consequences of the significant variability seen in the ordering patterns for common conditions such as chest pain, it is time to reevaluate how we develop and use diagnostic guidelines/pathways in healthcare.
Recognizing that health care is local, it is imperative to leverage approaches that involve health system laboratory and clinical thought leaders to design diagnostic pathways and change management processes that meet the needs of the local practice.
Conclusion
Variety is the spice of life. Reducing non–value-added variation in healthcare won’t make life less exciting. It can help to improve the patient and provider experience and reduce the cost of healthcare.
Resources mentioned in this article:
“Variety Is the Spice of Life,” Ginger Software, accessed November 7, 2020, https://www.gingersoftware.com/content/phrases/variety-is-the-spice-of-life/.
U.S. Preventive Services Task Force https://www.ahrq.gov/cpi/about/otherwebsites/uspstf/index.html
JAMA Open Network Cascades of Care After Incidental Findings in a US National Survey of Physicians, October 2019
https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2752991
Institute for Clinical Systems Improvement
U.S. Preventive Services Task Force
https://www.ahrq.gov/cpi/about/otherwebsites/uspstf/index.html
Additional Reading
The Community Clinical Laboratory of the Future
Shifting Focus From Lab Industry To Lab Medicine
Hospital Laboratory Outsourcing and its Unintended Consequences
Think Twice Before Selling Your Hospital Outreach Lab
