
Hospital Laboratory Outsourcing and Its Unintended Consequences
Hospitals and healthcare organizations are facing multiple challenges.
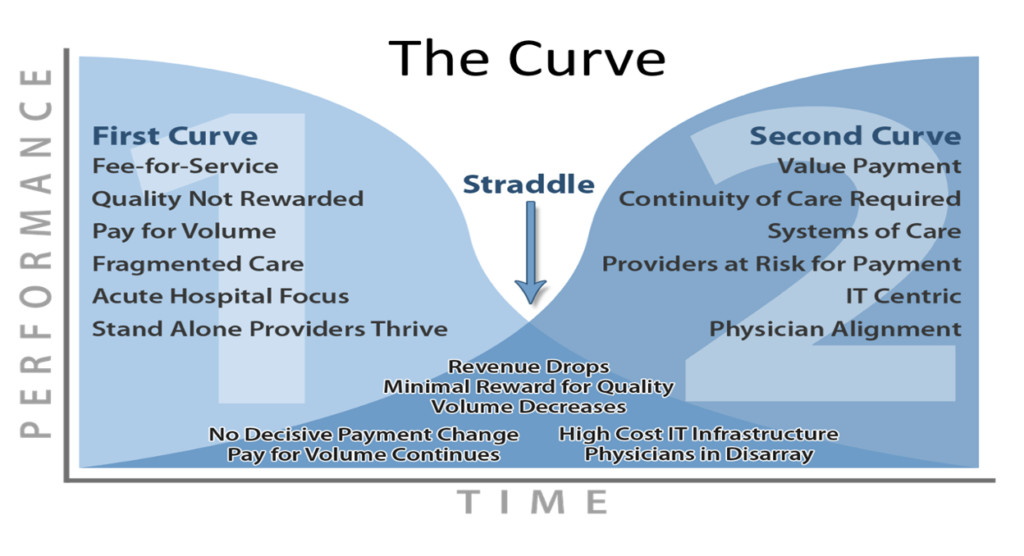
The transition from fee-for-service healthcare reimbursement to value-based care reimbursement as reflected below is at a difficult phase. Reimbursement from fee-for-service is declining more rapidly than the revenue is increasing from value-based care.
This situation compounded by the global pandemic has underscored the precarious financial state of many healthcare organizations. Thus, there is a growing need for these institutions to find new sources of profitable income, and efficiencies to enhance the net operating income from current activities.
Approximately half of U.S. hospitals finished 2022 with a negative operating margin per Becker’s Hospital CFO report, 01/30/2023
As a result of these financial pressures, outsourcing has become an increasingly common cost reduction approach employed by hospitals and healthcare systems.
Unintended Consequences
In a recent article “The High Stakes of Outsourcing in Healthcare” published by Leonard L Berry PhD MBA et al. in The Mayo Clinic Proceedings, the authors pointed out that this strategy can have numerous unintended consequences, including inconsistencies in standards of care, harmful medical errors, decline in patient and employee satisfaction, and damage to clinicians’ morale and income, as well as the healthcare organization’s culture, reputation, and long-term financial performance if these potential relationships are not carefully reviewed.
Specifically, the article explores the high stakes of outsourcing healthcare services that directly affect patient care such as emergency medicine, radiology, laboratory services, and environmental services, which are among the most commonly outsourced hospital services.
Implications
This review will focus on the implications of outsourcing the hospital laboratory services to national commercial labs. This growing trend is seen by many hospitals and healthcare systems as financially rewarding and a needed response to the current challenging environment.
However, numerous conversations with health system executives reveal that much of this outsourcing has likely occurred because the value of the hospital clinical laboratory and the associated opportunity costs are not fully appreciated. This knowledge gap stems from healthcare’s fee-for-service history where services were viewed in a siloed manner.
As a result of this compartmentalization, the links between the financial and clinical outcomes of different units were not widely considered. Consequently, clinical laboratory services were viewed as commodities rather than an integral infrastructure element supporting patient care delivery.
Transitioning to Value-Based Models
As healthcare transitions from fee-for-service to value-based and more broadly bundled reimbursement models, the laboratory’s important new role will become clearer.
The assertions outlined by the authors of this article are based on the following facts. The clinical laboratory:
- Represents only 3% to the healthcare expenditure in the United States while generating 60% to 70% of the information in the patient’s medical record, thus representing a significant untapped operational leverage
- Generates data that either triggers or confirms the vast majority of patient-related medical decisions
- Contributes information needed for every patient’s care in nearly every care setting
- Responsive to health system service needs, as a result the laboratory possesses capacity concerning its plant and equipment during off-peak periods
- Expand diagnostic capabilities associated with genomics and molecular diagnostics in support of the health system’s “personalized healthcare” initiatives targeting more efficient and effective local patient care
- Supporting the providers with access to cutting edge information concerning these new technologies and in meeting their demanding schedules from a diagnostic workflow perspective
Due Diligence
Clearly, outsourcing this critical clinical service requires careful consideration. In their article, Dr. Berry and colleagues outlined the following key questions which health systems should diligently consider before establishing an outsourcing relationship:
- Will our patients benefit?
- Will we enhance patient safety?
- Will our employees benefit?
- Will our third-party payers benefit?
- Will we strengthen our overall capabilities as we pursue a broader organizational strategy?
- Will we increase our organization’s flexibility and innovation?
- Will we bolster our organization’s reputation brand?
- Will we improve our long-term, not merely our short-term, financial performance?
Before we propose our answers to these questions as they relate to the outsourcing of clinical laboratory services to commercial laboratories, it is important to emphasize that the vast majority of commercial labs strive to provide quality services to hospitals and healthcare systems.
However, their core operating model is focused on cost reduction through economies of scale regarding testing in isolation leaving the health system to deal with the increased episode of care costs caused by delays as patient specimens leave the community.
This model worked reasonably well in the fee-for-service environment, however, in our opinion, it will not meet health system needs in a value-based care reimbursement environment.
Our Answers
Our answers to the questions posed by Dr. Berry and his co-authors are given in the context of outsourcing of clinical laboratory services in a value-based-care environment.
- Will our patients benefit?
Probably not.
>>> Outsourcing clinical laboratory services has the potential to extend turn-around times for tests which are aggregated at remote high-volume testing sites. Under this model, patients’ samples leave the community to achieve economies of scale, causing results to potentially be delayed by one to two days.
- Will we enhance patient safety?
Probably not.
>>> Due to the aforementioned delays, providers will not receive all the required information in a timely manner, which may compromise patient safety. In addition, transporting samples over long distances increases the probability of loss (requiring sample recollection) or decrease specimen integrity (which could lead to spurious results), causing further patient inconvenience and/or even potential harm.
- Will our employees benefit?
No.
>>> Generally, when laboratory services are outsourced, clinical lab employees are either laid off or do not find the work as rewarding as their previous roles. In addition, nursing and medical staff are often frustrated by the delays in service and a general lack of response from the vendor when questions arise.
- Will third-party payers benefit?
Yes and No.
>>> Although they will likely receive somewhat lower test prices, the aggregate cost of care will likely increase due to the previously identified delays and lack of alignment between testing protocols and local patient care pathways. Therefore, payers may benefit from more affordable laboratory services, but this saving will be far outweighed by the non-lab aspects of care.
As a reminder, laboratory services represent approximately 3% of the total cost of care, but generate 60% to 70% of the data impacting patient care decisions. If these negative impacts are avoided by keeping the testing local, a relatively small increase in the laboratory costs will be eclipsed by the “savings” seen concerning the episode of care costs.
- Will we strengthen our overall capabilities as we pursue a broader organizational strategy?
Probably not.
>>> As the health system’s control over this core service diminishes, its ability to tailor services to local needs will inevitably decline. Therefore, outsourcing to vendors that generate profit from testing in isolation is not aligned with the core health system objective, i.e., managing the aggregate costs of care.
- Will we increase our organization’s flexibility and innovation?
No.
>>> If hospital clinical lab testing work is outsourced, the potential for innovation is vastly reduced. In addition, flexibility in diagnostics workflow processes are also constrained because the outsourcing vendors primarily achieve economies of scale only if there is consistency across their national client base.
The clinical laboratory represents a highly valuable, yet underutilized, tool in the hospital’s innovation toolbox. Hence, outsourcing the clinical laboratory services will compromise health system leadership’s ability to fully benefit from this potential innovation should the health system focus shift from viewing the lab as a cost silo to a core element impacting episode of care costs.
- Will we bolster our organization’s reputation and brand?
Probably not.
>>> The services in question are not provided by the local institution, hence there is a real risk of adverse impacts to the service levels which could damage the organization’s brand.
- Will we improve our long-term, not merely our short-term, financial performance?
Probably not.
As Dr. Berry and his colleagues commented in their article:
“although the primary goal of outsourcing is cost efficiency, resulting financials often do not meet expectations, especially if the indirect cost of lowering quality are accurately accounted as contributing to poor outcomes such as medical errors, loss of employees trust, and increase hospital readmissions.”
The evidence provided by Barry, etal, further indicates that, over time, hospitals in outsourced relationships often experience unplanned cost increases associated with test price increments and lack of control over test utilization, resulting in excessive and high-margin testing, and unsustainable management fees.
As a result of these adverse consequences, two hospitals included in this review ended their outsourcing arrangements and reported immediate first-year savings of $1 and $4 million dollars, respectively once the relationship was terminated. In our opinion, this financial impact is further complicated when the reduction in potential for profitable incremental lab revenue is taken into account.
Fortunately, there are alternatives to the outsourcing of this valuable component of the local healthcare delivery system while still addressing the growing financial challenges faced by the organization. These strategies focus on growth, enhanced service delivery, and the local practice of laboratory medicine with the aim of reducing aggregate episode of care costs. The clinical laboratory can play a central role in achieving these goals.
Understanding the Strategic Value
How can health system leadership begin this journey to gain a greater understanding of the potential and strategic value embedded in a clinical laboratory?
First, it is important to recognize that the majority of benefits generated by the lab reside outside the lab. These benefits need to be quantified and taken into account when making strategic decisions regarding the lab and the community’s diagnostic pathways and processes.
Second, since the strategies for reducing costs in a value-based-care are almost opposite of those designed to reduce costs under fee-for-service reimbursement, new health system operational models will be required. In the authors’ opinion, hospitals and healthcare systems should pursue the integration of laboratory diagnostics across the community’s continuum of patient care.
In Summary
An effective and efficient community healthcare system requires an efficient and effective clinical laboratory as an integrated local partner. For this collaboration to yield its maximum benefits, the laboratory must grow and expand in scope.
Leveraging laboratory expertise as a core competency across all service lines and community care settings represents a significant opportunity to position community health systems for:
- value-based at-risk reimbursement environment
- incremental revenue and margin generation in support of the health system’s mission
Pathologists and laboratorians should redefine their valuable role within the context of the patient’s episode of care. They also need to work with health system leadership to ensure that appropriate strategic decisions regarding the health system are made in consideration of the significant value that the clinical labs can deliver.
- Labacoeconomics™: Expanding the Role of Clinical Laboratories in Value-Based Healthcare - February 26, 2024
- Pace of Hospital Lab Acquisitions Likely to Remain Steady - April 29, 2023
- Measuring Clinical Laboratory Contributions - April 29, 2023
